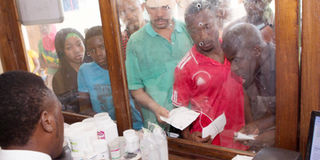
Dar es Salaam Whenever a patient is told that medicine is out of stock at a public health facility, the same questions arise: Who is responsible and why does the problem persist despite increased government spending on health services?
This concern continues to plague many citizens, especially at a time when the government has promised to improve access to medicines across the country.
In a recent interview in Dodoma, Chief Government Pharmacist Daudi Masi gave a detailed account of how the health commodity supply chain operates, from the dispensary level to the national level, and where breakdowns can occur.
The supply chain starts at the facility level
According to Mr Musisi, the availability of medicines does not start at the Ministry of Health or the Medical Stores Department (MSD), but at individual health centres.
Every year, more than 8,000 health centers across the country prepare drug forecasts from August 1 to December 31. During this four-month period, health workers collect data on patient numbers, disease trends, and drug use to estimate demand for the coming year.
“The system uses modern technology known as Electronic Logistics Management Information System (eLMIS), through which all facilities present their requirements digitally,” he explained.
No facility is allowed to submit requests outside the system, a move aimed at increasing transparency and accountability.
However, this raises a key question: Do frontline health workers have the ability to make accurate predictions?
A multi-level review process
Mr. Massey said once the establishment submits its forecasts, the data goes through several stages of review – at the council, regional and finally national level through the Office of the President – Regional Administration and Local Government (Tamimi).
At each stage, estimates are scrutinized, adjusted and adjusted to available funding. They are then submitted to the National Drug Forecasting Committee, headed by the Chief Government Pharmacist.
“We receive national demand estimates, analyze them and ensure they reflect reality before sending them to MSD for implementation.” he said.
Still, the many layers of review raise other concerns about whether actual requirements may change or diminish along the way, ultimately affecting drug availability.
Funding gaps lead to shortages
After approval, the next step involves planning for procurement and distribution, which is done jointly by the Ministry of Health, Tamimi and MSD.
This step assesses the level of available reserves against the estimated requirements for the year. However, a major challenge arises when available funds fall short of actual requirements.
“When there’s a gap between financing and actual demand, that’s where another source of shortages starts,” Mr Massey noted.
MSD roles and health facilities
Once funds are secured and drugs are received, MSD is responsible for distributing to health facilities based on recommendations every two months.
Healthcare facilities, in turn, must submit timely and accurate orders based on their needs.
If MSD fails to deliver, it is liable. However, if the facility makes errors in forecasting or fails to plan properly, accountability shifts to facility staff and local government officials.
“It’s a chain involving many players, each with their own responsibility,” Mr Massey stressed. Yet, for ordinary citizens, such explanations may offer little comfort when medicine is not available.
A pharmacist dispenses medicine at a public health center. Every year, more than 8,000 health centers across the country prepare drug forecasts from August 1 to December 31. PHOTO | file
The government has invested in digital systems to improve medication tracking. In addition to eLMIS, health facilities use electronic medical record systems.
The goal is to integrate these platforms to provide real-time data—from the time drugs enter the system to the time they are dispensed to patients.
“We aim to get to a point where within minutes we can identify which facilities are deficient and take immediate action,” he said.
Artificial intelligence is also being introduced to enhance forecasting accuracy.
However, questions remain as to whether technology alone can solve deep structural challenges such as shortages of skilled personnel and limited financial resources.
Shortage of professionals
A significant challenge facing the health sector is the shortage of qualified personnel, especially pharmacists.
As a result, medication management is often handled by nurses or laboratory technicians, which can affect the quality of decision-making.
Mr. Mousasi said, the government has started to eliminate this gap by hiring 12,000 health workers in the current financial year.
“We also provide extensive training. Our teams are field support staff – often you’ll find a nurse or lab technician to help with forecasting and stock verification,” he said.
“We believe that having the right professionals, as the government continues to do, will be a key solution in mitigating this challenge.”
Losses of termination are incalculable
Despite advances, the availability of medicines remains an insurmountable challenge, especially in countries that rely on imports.
“You have to prepare for illnesses even if they don’t happen. If they don’t happen, the medicine goes unused and expires,” explained Mr. Massey.
He stressed, however, that performance is measured by the price of expired drugs. Tanzania’s rate is currently two percent below the international benchmark of five percent.
“In the 2024/2025 financial year, the number of expired drugs is estimated at 0.9 percent, which is much less than the previous level,” he said.
However, for citizens facing shortages, even such figures may be significant.
“It is impossible to run out of drugs in the facility or MSD warehouses because we buy in anticipation of diseases. If an outbreak like cholera does not occur, some drugs will run out,” he added.
Deviance and accountability
Mr Masi also acknowledged the problem of drug diversion, with reports indicating cases of theft and misuse involving some health workers.
Strong monitoring systems are in place, including internal and external audits and cooperation with agencies such as the Prevention and Combating of Corruption Bureau (PCCB), he said.
“When the medicine does not reach the patients, audits are initiated through audit units and monitoring agencies such as the Comptroller and Auditor General (CAG),” he said.
“There are ongoing cases in the courts where employees are accused of transporting drugs or medical supplies. Some have been convicted, while others are facing legal action. The PCCB plays an important role in ensuring accountability.”
In situations where medicine is not available in public facilities, patients are often forced to buy it from private stores at their own expense.
This increases the financial burden, especially for low-income families.
The government hopes that the implementation of universal health insurance will help alleviate this pressure by ensuring access to services without out-of-pocket payments.
A closer look shows that there is no single cause of drug deficiency. This issue has a complex chain that involves health workers, local authorities, regional administrations, ministries, MSD and even the Ministry of Finance.
Mr Massey said when any link in this chain fails, the impact is ultimately felt by the patient.
He suggested that perhaps the most important question is not who is to blame, but how the system can be strengthened to ensure the continued availability of drugs.
Because, in the end, public health cannot wait for administrative solutions.
#drug #shortages #persist #Tanzania #major #health #reforms