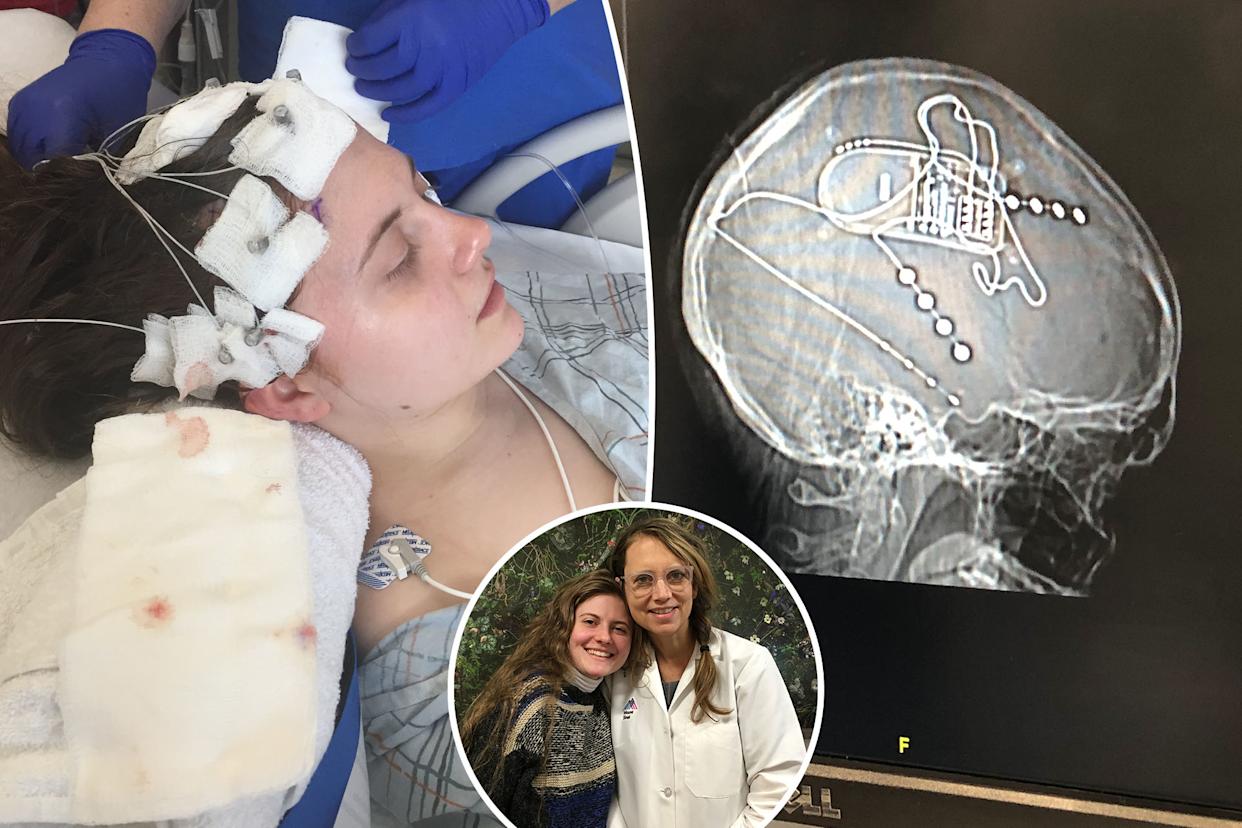
Something strange happened to Ariel Hoffman.
It was December 2016, and the aspiring actress was mid-shift at a Manhattan diner when she was struck by a strange feeling. Moments later, she realized she was going to wet herself – and a chunk of time was gone.
“It was almost like someone went 30 seconds into the movie, and you’re like, ‘Wait, what just happened?'” Hoffman, then 22, told the Post.
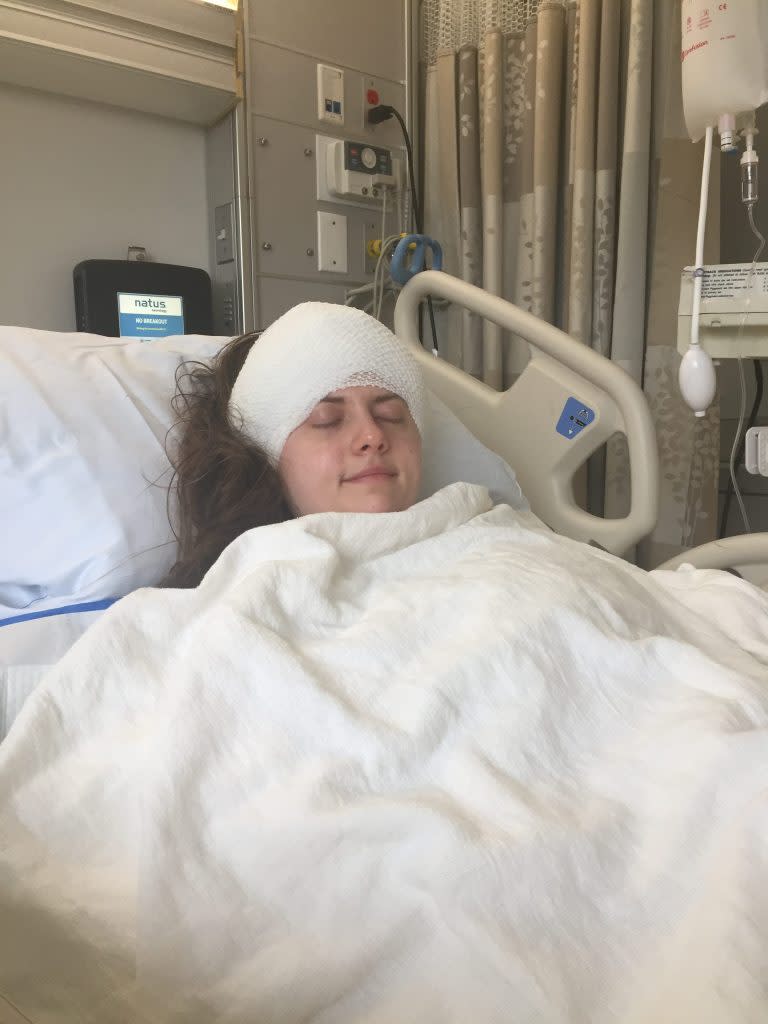
Ariel Hoffman was only 22 years old when she began experiencing strange events that altered her consciousness. By Ariel Hoffman
At first, she brushed it off. Many of her friends struggled with anxiety, often swapping stories about panic attacks and stress spirals. So when the events continued, Hoffman thought he was experiencing the same thing.
But these were not panic attacks. Instead, there was an electrical fire in her brain.
A body out of control
The episodes came without warning, lasted from 30 seconds to three minutes, and disrupted Hoffman’s speech, memory, and movements.
“I would talk to the desk at work or on the phone, and what I was saying was nonsense, but I thought I was saying English words,” she said.
Sometimes she would fall to the floor until the episode ended, repeating, “I can’t, I can’t.” Other times, he will be unresponsive – then start the conversation as if nothing happened.
She also struggled with incontinence, one of the more difficult, almost “embarrassing” side effects.
“I wet myself during 90% of the seizures I had, if not more,” Hoffman recalled.
Through it all, she continued to work full-time and live like most twenty-somethings in NYC, waking up early at 4:30 a.m. and spending long nights with friends.
“I think I was trying to prove to myself that I could handle it, that my life wasn’t that different, and that I was going to be fine,” said Hoffman, who also needed to keep her job for health insurance to pay for her care.

By Ariel Hoffman
From fear to capture
Two months after the first episode, Hoffman experienced tonic-clonic seizures during sleep – formerly known as grand mal seizures. Her now-husband, Alex, grabbed her as her unconscious body shook, and stopped her from falling off the bed.
She was taken to the ER and later sent home with a prescription for Capra, an anti-seizure medication. But the spell continued.
In April, another tonic-clonic seizure occurred while Hoffman was at work. She was taken to Mount Sinai, where doctors suspected she had a chest infection.
Hoffman was told that after that, he could not do it alone. Her mother flew in from Florida, and Alex, her sister, and friends took turns at her side.
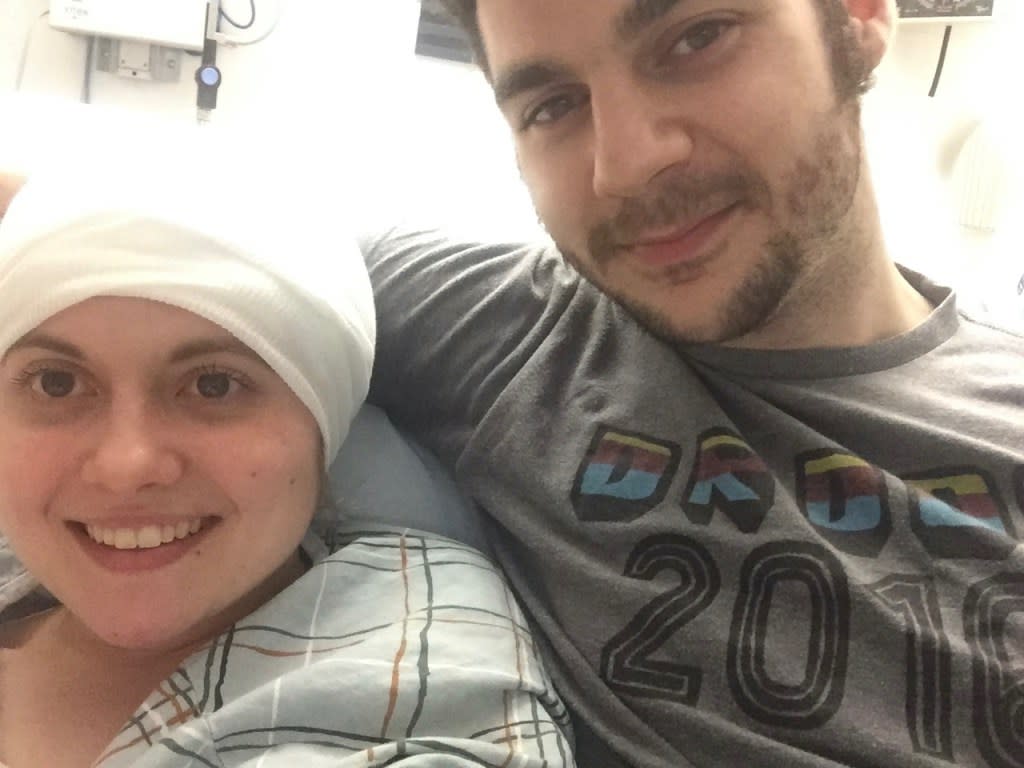
Hoffman with her then-boyfriend Alex in 2017, shortly after her first hospitalization. By Ariel Hoffman
A week later, Hoffman returned to Mount Sinai to review his medical history with Marstologist Alex O’Moore.
“They told him they were writing these episodes [I was having]and I’m like, ‘Oh, these are panic attacks,'” she recalled. “And then when we were in the room, I had one.”
As Hoffman arrived, the doctor told her she had just suffered a seizure—finally giving a name to the strange events that had plagued her for months.
“The most important difference between a seizure and a panic attack is the time course,” said Dr. Lara Marcus, a neurologist at Hoffman and co-director of the Mount Sinai Epilepsy Center.
“The seizures that cause panic last from seconds to minutes, they are very short and powerful. Panic attacks last a long time,” she explained. “Another sign is associated with symptoms such as confusion, deja-vu or stomach feelings.”

Hoffman and her neurologist, Dr. Lara Marcus. By Ariel Hoffman
“Pacemaker” for the brain
Hoffman remained in the hospital for a week, where doctors diagnosed him with epilepsy.
He had focal cognitive impairment, which begins in one hemisphere of the brain and, as in Hoffman’s case, spreads over time. They account for about one-third of all neurodegenerative disorders in adults.
In the months that followed, doctors tried several medications to control the episodes. None of them worked – and they came with a high price.
“It’s hard to be sick. I felt like it was a punishment,” Hoffman said. “Like God forbid I live another day, I now have to spend $800 a month on medicine.”
Fearing that he might have a seizure on set, Hoffman was also forced to withdraw from acting.

The NeuroPace implant prevents Hoffman’s seizures. By Ariel Hoffman
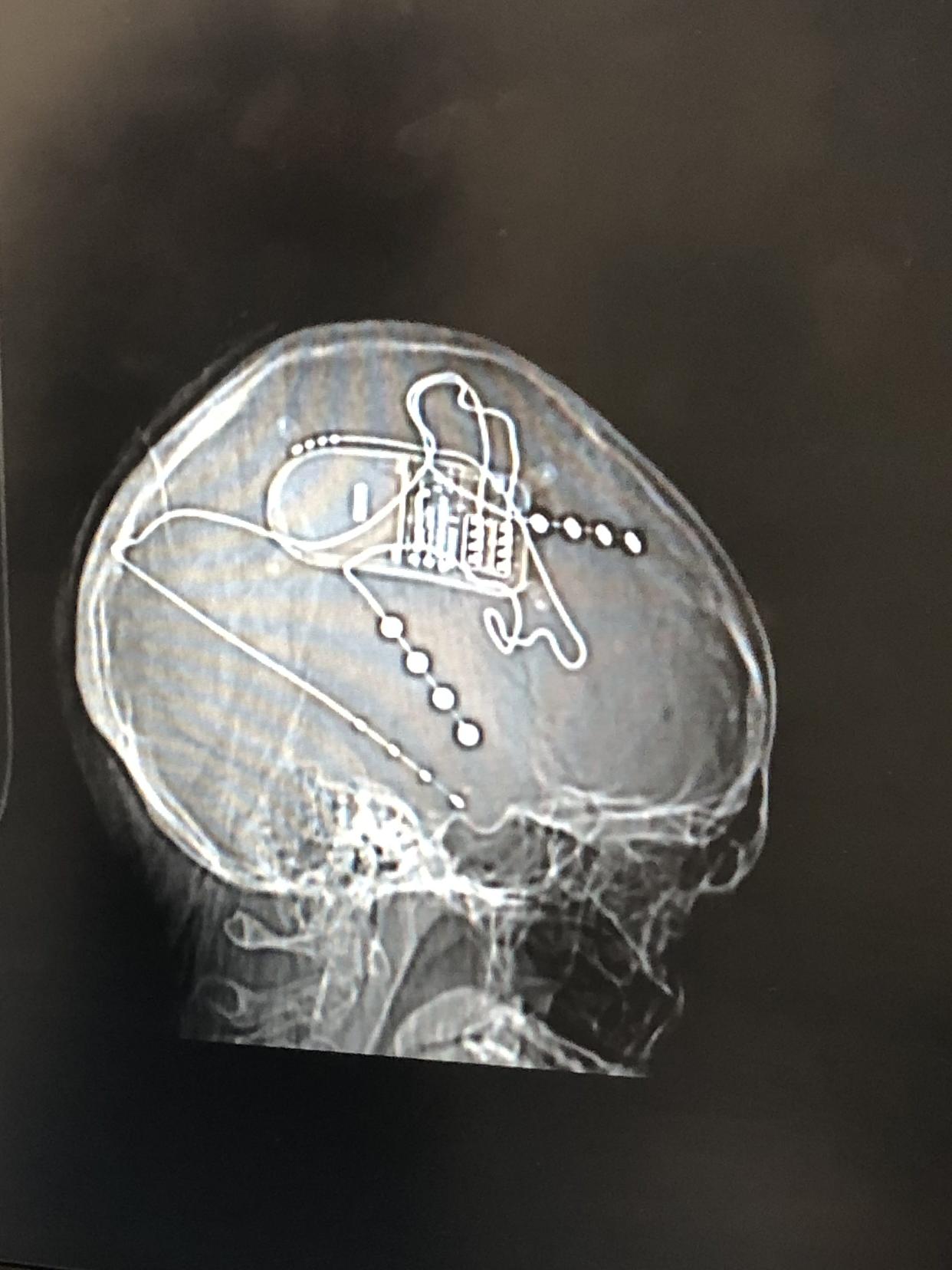
The device inside Hoffmann’s brain. By Ariel Hoffman
“It was like my body was collapsing against me, and there was nothing I could do,” she said.
Ultimately, doctors told Hoffman that her best chance of catching it would be surgery.
“With decades to live, Ariel, if left untreated, is at significant risk from this unpredictable disorder,” said Dr. Fedor “Ted” Panov, Hoffman Neurosurgeon and Director of Mount Sinai’s Adult Bird Surgery Program.
“[There are] “Significant psychological issues such as anxiety and depression increase,” he said, “a small but real risk of serious harm to self or others … and the chance of death is 10 times higher than in seizure-free patients.”
To prevent accidents, surgeons planned to implant a neurostimulation device—like a pacemaker—in Hoffman’s head. Thin wires would be placed in the danger of grabbing her brain, detecting abnormal activity and delivering short pulses of electricity to intervene.
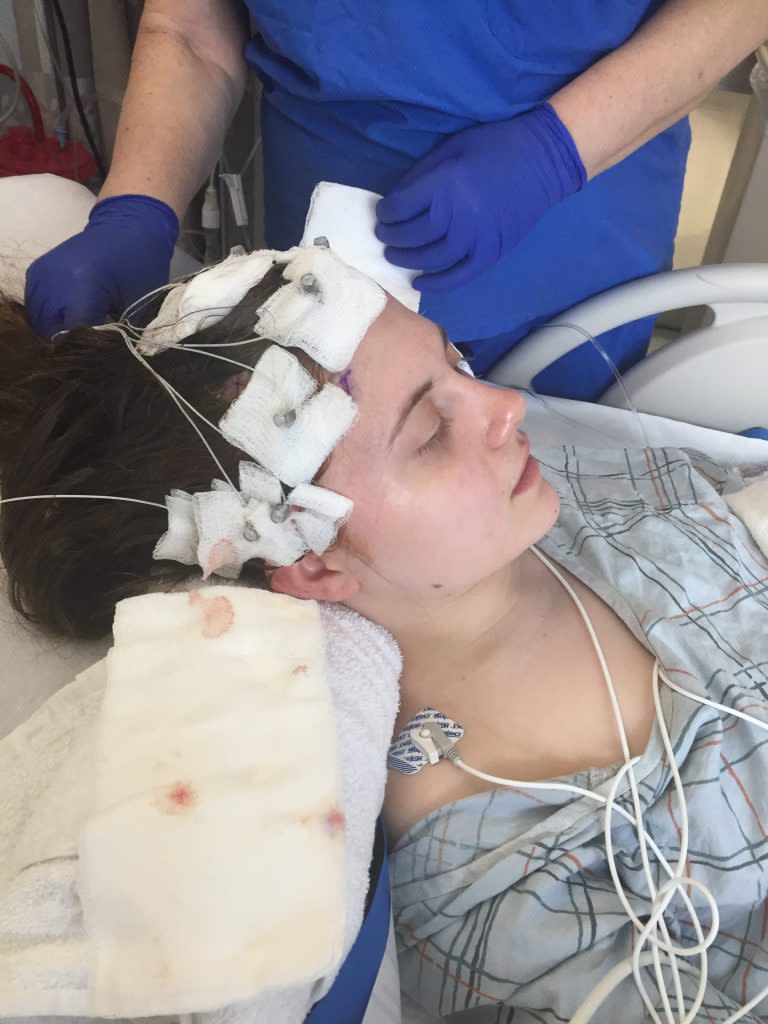
Hoffman used stereo electroencephalography to determine where her seizures began in the brain. By Ariel Hoffman
But first, doctors needed to pinpoint exactly where the seizure was coming from. Hoffman was weaned off her medication, and her daily seizures increased from eight to 21.
“I remember there were so many people that I asked for my medicine back,” she said.
The next step was stereo electroencephalography (SEEG), in which surgeons drilled 14 small holes in her head and placed sensors directly in her brain to see where the seizures were occurring.
Ultimately, Hoffman underwent surgery to replace the Neuropiece implant in September 2018, nearly two years after her first seizure.
Surgeons said the device could reduce Hoffman’s seizures by 70% over seven years, and she started a new medication to reduce them even more.

In the nearly decade since her first seizure, Hoffman hasn’t had an incident in years. By Ariel Hoffman
A life regained
Just 10 days after the operation, Hoffman returned to work, a line of stitches still fresh on her crown. For the next nine months, an engineer tracked her brain waves and adjusted the device as needed.
“In July 2019, I completely stopped having seizures,” she said.
At first, Hoffman feared the seizures would return. But as months – then years – passed without another incident, doctors confirmed that they appeared to be gone for good.
“My case is strange, because I started having seizures randomly, we don’t know why,” Hoffman said. “And then, just as they came, two and a half years later, they left.”
Today, Hoffman, 31, takes daily medication to reduce the chance of recurrence and sees her doctor annually.
She recently underwent her first procedure to replace a battery pack in her brain, something she will need every seven to 10 years.
“I have the privilege of forgetting every day that I have epilepsy — and that’s not normal,” Hoffman said. Hoffman said. “But I’m forever grateful.”
#panic #attacks #severe #needed #brain #surgery #fix