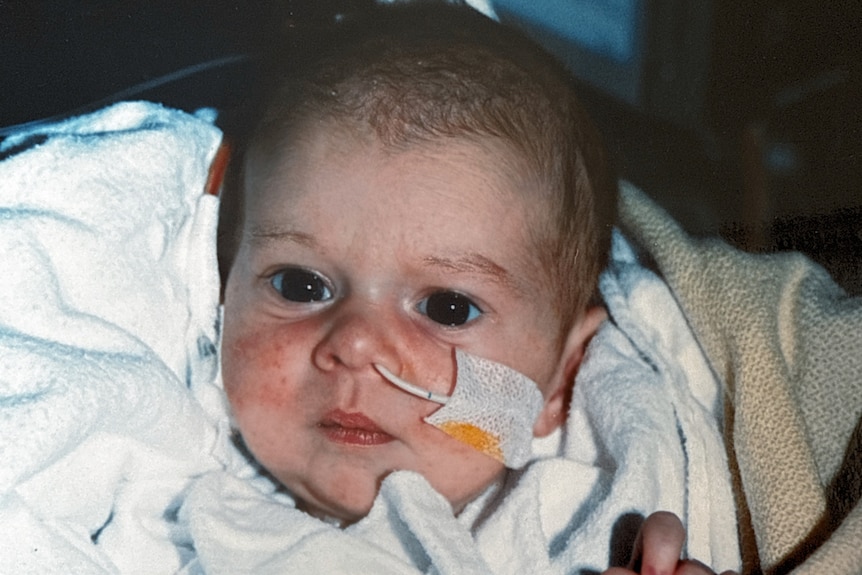
Ryan Bowman has faced many health battles in his 33 years.
Born with five congenital heart defects, he underwent four surgeries, the last of which left him with a brain injury.
Dubbed a “miracle child” in an article in the Adelaide Advertiser, he persevered through his teenage years to get his driver’s license and became a father in his 20s.
In 2023, he was diagnosed with Hodgkin lymphoma but, after intensive chemotherapy, celebrated the entry of immunity.
Ryan Bowman was born with five congenital heart defects. ((Presented by: Deb Brooks)
“He loved his friends, he loved his brothers, and he especially loved his nieces and nephews, and of course, his daughter,” said Ryan’s mother, Deb Brooks.
said
“After he got the brain injury, it was rehabilitation, he had to learn to walk, talk, see.
“That kind of stayed with him all his life.”
A year after entering remission, Ryan was diagnosed with end-stage heart failure.
On February 15, 2025, he was admitted to Mount Gambier and District Health Services.
“Ryan was admitted very ill on Saturday morning, he had a chest x-ray and was diagnosed with double pneumonia,” Deb said.

Ryan has been a lifelong supporter of the Adelaide Crows. ((Presented by: Deb Brooks)
As his condition worsened, Ryan’s admission became a palliative care case, which both his mother and an independent report had fallen short of expectations.
“One of our big things was not to talk in front of Ryan and they did,” she said.
“They talked about ‘this could be life-ending’, things like that.”
Attention deficit and neglect phobias
Deb and Ryan’s stepfather, Chris Brooks, knew Ryan’s basic health diagnoses “like the back of their hand” and kept a scrap of paper to help paramedics and hospitals when Ryan needed care.
“In hindsight, if Ryan or someone like Ryan delivered to Mount Gambier Hospital today, Mount Gambier Hospital wouldn’t see another Ryan for 200,000 years; that was bad luck.”
Chris said.

Ryan was diagnosed with Hodgkin lymphoma, but fought through chemotherapy and entered remission. ((Presented by: Deb Brooks)
Chris said that information provided by himself and Deb, such as Ryan’s fear of needles, was ignored and led to a situation where a tray of needles was placed in his stomach before the drug was administered.
“We made it clear that if any life-ending medication is given, it should go through his cannula so that he doesn’t experience any more pain, if you will,” he said.
“It didn’t happen.”
The independent review, carried out by the director of palliative care at St Vincent’s Hospital in Melbourne, Professor Mark Bogie, found a number of failings in Ryan’s care.

Deb and Chris say they want to help create better palliative care outcomes for local families. ((ABC South East SA: Josh Breen)
The report states that at 1:30 a.m., Ryan’s condition changed significantly and the nurses called the doctor at 4:30 p.m. to review the patient.
This doctor’s review was conducted at 7am, which report noted “recognition of significant impairment in retrospect appears to have been delayed and delayed”.
Another review around 9:30 a.m. led to a change from stable to palliative care, but pain relief was not administered until 1:30 p.m.
Ryan died shortly after.
Professor Bogie’s report also found that Ryan’s family’s wishes and knowledge of his condition were often ignored, despite their long-standing role in his care.

A memorial to Ryan at Chris and Deb’s home. ((ABC South East SA: Josh Breen)
“After Ryan’s death, and in discussions with his family, d [Limestone Coast Local Health Network] LCLHN conducted an external clinical review to independently assess the care provided to Ryan at Mount Gambier and District Health Services,” said LCLHN CEO Emma Poland.
“LCLHN has accepted the review’s findings and recommendations and is committed to implementing them as part of our health service quality improvement processes.”
Hospitals need to rethink
Flinders University palliative care expert Claudia Verdon said it was common for families to be unaware of the palliative care their loved one was receiving in hospital.
She said modern medicine means patients with complex health conditions tend to live longer, making specialist care more important.

Claudia Verdon says hospitals need to rethink how they deliver palliative care. ((ABC News: Daniel Taylor)
“Our hospitals in Australia are really well set up to support people who have acute and episodic concerns that are treatable,” she said.
“But we are not well-equipped to care for people who are now living with many serious illnesses that cannot be cured.“
Providing palliative care specialist training to health care workers will create better experiences for patients and families, Dr. Verdon said.
“Training is the first step, but we really need better systems in our health environment to put that training into practice,” she said.
“We can often learn about what is best, safe, evidence-based care, but in some of our systems and structures delivering that is not always as straightforward as it needs to be.”
Educating the next generation
Ryan’s family has spent the year since his death planning a foundation to promote better end-of-life care in hospitals.
They launched the Ryan Bowman Legacy of Care Foundation, which will award scholarships to health professionals to pursue further studies in the field of palliative care.
The foundation will first offer scholarships to health workers on the Limestone Coast, and plans to expand to the rest of South Australia.

Ryan (middle) with his brother, Lachie and his mother, Deb. ((Prepared by: Chris and Deb Brooks)
“When a family member presents to a facility with a very sick child, parent, child, whatever the case may be, it’s usually the first time the clinician has seen that person,” Chris said.
“We feel like there needs to be a mesh between that caregiver, the parent, and the center of that mesh for that individual’s ongoing treatment.”
The charity has partnered with the US-based DAISY (Diseases Attacking the Immune System) Foundation, which has run an international program to recognize nurses since 2000.
Bonnie and Mark Barnes started the foundation after the death of Mark’s son, Patrick, and has identified nearly 4 million nurses worldwide, developing instructional programs for patient-centered care for use in medical facilities.

Mark and Bonnie Barnes say that recognizing good health care leads to better patient outcomes. ((Provided by: The DAISY Foundation)
“What happens when you have an organized way of celebrating all the good things that are going on, it really changes the culture,” Ms Barnes said.
“We see cultures that are inspired with gratitude, that become more innovative, where compassion, fatigue and burnout are reduced as a result of being recognized or nominated for an award like this.
“There are many benefits to nurses and their organizations and to patients who prescribe to having a culture where meaningful recognition prevails.”
Throughout Ryan’s life, Deb kept a detailed journal of his health struggles, personal milestones, and her thoughts while traveling.
In hundreds of hospital visits throughout his life, Ryan was seen by dozens of doctors, nurses and paramedics.

Deb has put nearly three decades of journal entries into a book that is expected to be released. ((ABC South East SA: Josh Breen)
Deb said her son has made some great connections with healthcare workers.
“I think with end-of-life care, you only get one chance to get it right.”
Deb said.
“Because you know, working with families, we’ll always remember what you did, but we’ll never forget what you didn’t do.”
#Ryans #young #life #family #abandoned